By Wang Cong
The expanding field of cancer immunotherapy has largely benefited from the success of adoptive T-cell therapy and/or checkpoint inhibition therapy in a small subset of patients with cancers that have failed conventional treatments (radiotherapy, chemotherapy, and surgery). However, the majority of cancer patients still exhibit poor responses to cancer immunotherapy, which may be attributed to genetic or epigenetic alterations in tumor cells, environmental factors, lack of adequate tumor-specific T cells, and the exhaustion phenotype of tumor-infiltrating lymphocytes (TILs). All these factors are decisive, implying that a deeper understanding of these mechanisms should be sufficient to accurately predict an individual's response or resistance to cancer immunotherapy.
However, the reality is that for patients with very similar disease conditions, cancer immunotherapy demonstrates significant efficacy in some individuals but is almost ineffective in others. Even in mouse models with identical genetic profiles, there are substantial variations in the response to cancer immunotherapy. Notably, multiple tumors derived from the same tumor clone implanted in the same mouse exhibit differing responses to cancer immunotherapy.
This suggests that there may be an inherent randomness in cancer immunotherapy, implying that even if we fully understand all known deterministic mechanisms in the future, this intrinsic randomness sets a theoretical upper limit for the success of cancer immunotherapy, rendering it impossible to completely predict treatment outcomes.
On February 5, 2026, researchers from the National Cancer Institute (NCI) published a research paper titled 'Stochasticity in cancer immunotherapy stems from rare but functionally critical Spark T cells' in the internationally renowned academic journal Cell.
This study demonstrates that the variability in cancer immunotherapy efficacy stems from a highly rare yet functionally critical T cell subset—Spark T cells.

The Mystery of the "Randomness" in Immunotherapy
In this study, the research team designed a sophisticated experimental system to simulate the immunotherapy process in a culture dish. They established thousands of identical experimental conditions, with each well containing the same number of cancer cells and T cells.
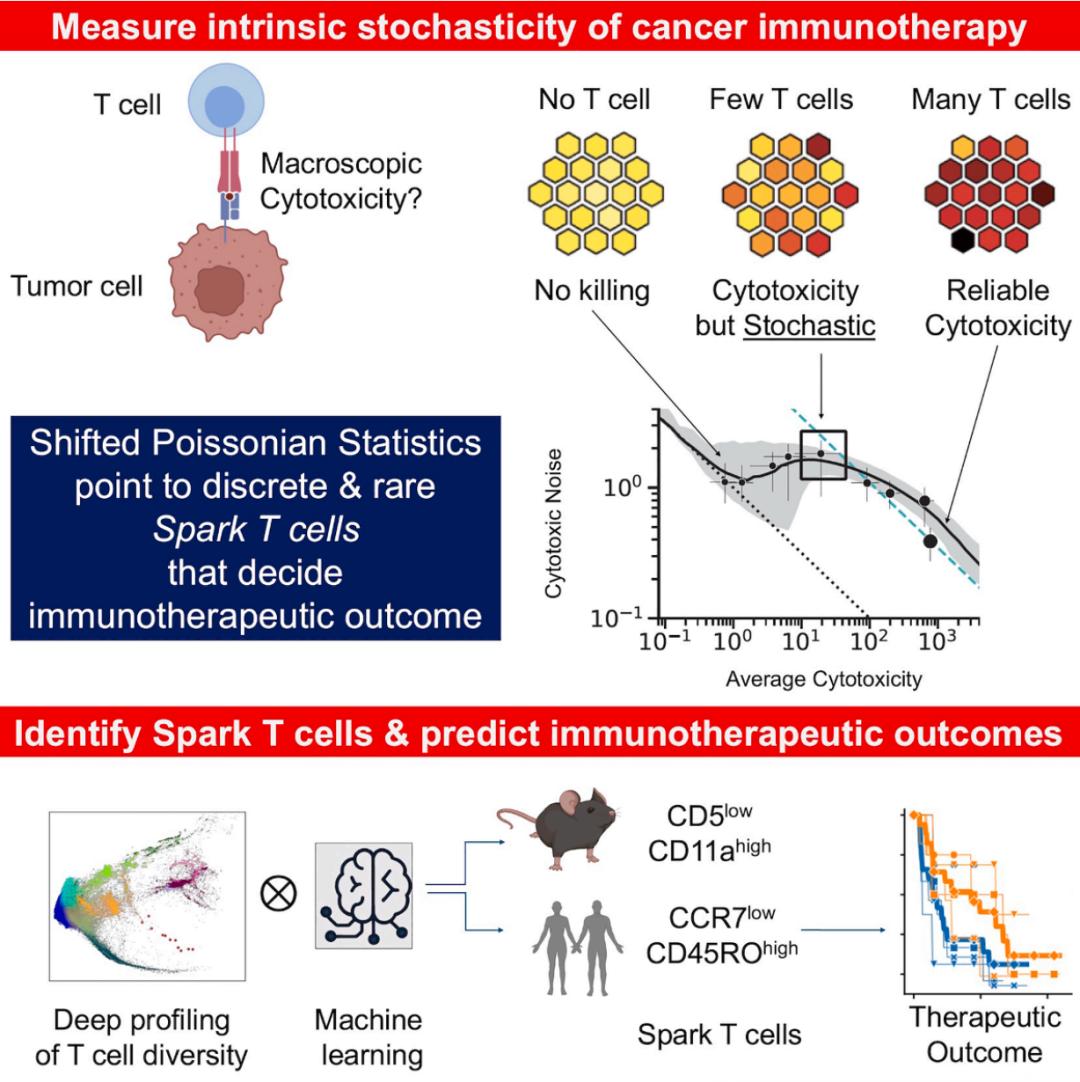
Surprisingly, even with identical initial conditions, the outcomes exhibited significant variations—cancer cells in some culture wells were completely eradicated, while those in others remained largely unaffected. These results indicate that immunotherapy demonstrates higher randomness (consistent with a biased Poisson process) compared to chemotherapy.
The research team further discovered that this randomness originates from differences in the activation phase of T cells. In certain responses, T cells are extensively activated and secrete large amounts of interferon-gamma (IFN-γ); in other responses, T cells remain almost entirely in a 'silent' state.
Discovery of "Spark T cells"
The research team predicted through mathematical modeling that this randomness might originate from an extremely rare subset of T cells—Spark T cells (spark T cells). They developed a single-cell stochasticity analysis workflow named Sto/CS, successfully identifying this critical group of Spark T cells from millions of cells.
The results demonstrated that Spark T cells constitute only 1/2500 to 1/1000 of all T cells. Upon recognizing cancer cells, these cells rapidly produce large quantities of IFN-γ, which subsequently activates more surrounding T cells through a positive feedback loop, ultimately forming a large-scale immune attack against cancer cells. A small spark can ignite a prairie fire—just one Spark T cell is sufficient to initiate the entire anti-tumor immune response.
To put it simply, the tumor-killing effect of T cells can be likened to a chain reaction of firecrackers. Spark T cells act as the initial spark, which randomly ignites subsequent firecrackers (this randomness stems from the stochastic activation of Spark T cells and the IFN-γ-driven positive feedback chain reaction). The statistical distribution of this process follows a shifted Poisson process.
Unique Properties of Spark T Cells
Why are Spark T cells so highly efficient? The research team discovered that these cells exhibit unique epigenetic features even in a resting state, particularly with the chromatin at the IFN-γ gene locus being in an 'open' state, enabling rapid response to antigen signals.
In mouse models, Spark T cells exhibit the CD5low CD11ahigh phenotype, whereas in human T cells, they display the CCR7low CD45ROhigh characteristics. These phenotypic features enable researchers to isolate and enrich these highly efficient T cells.
More importantly, the research team discovered that the abundance of Spark T cells was directly correlated with the efficacy of immunotherapy. After analyzing extensive clinical data, they confirmed that the more prominent the characteristics of Spark T cells in tumors, the better the patients' response to immune checkpoint inhibitors (particularly anti-CTLA-4 therapy).
Clinical Significance and Future Prospects
This finding holds significant implications for improving cancer immunotherapy:
First, detecting Spark T cell markers in tumor samples may emerge as a novel biomarker for predicting the efficacy of immunotherapy. Physicians can evaluate whether patients may benefit from treatment prior to administration, thereby avoiding the side effects and financial burden associated with ineffective therapies.
Secondly, enrichment or expansion of Spark T cells may represent a direction for the next generation of cell therapies. By increasing the proportion of Spark T cells in therapeutic products, the efficacy of adoptive T-cell therapy could be significantly enhanced.
This study provides a novel framework for understanding the variability in immune therapy responses. In the future, by modulating these key cellular subpopulations, it is expected to transform the efficacy of immunotherapy from a random, luck-dependent approach into a more controllable and effective method.
Paper link:
https://www.cell.com/cell/abstract/S0092-8674(25)01439-4
Disclaimer: This article is intended solely for knowledge exchange, sharing, and popular science purposes, and does not constitute commercial promotion, nor should it be regarded as medical guidance or medication advice. For copyright infringement, please contact us for removal.
Our product recommendations:
1.37042-63-0 https://www.bicbiotech.com/product_detail.php?id=6517
2.349438-38-6 https://www.bicbiotech.com/product_detail.php?id=6518
3.1629908-92-4 https://www.bicbiotech.com/product_detail.php?id=6519
4.281224-40-6 https://www.bicbiotech.com/product_detail.php?id=6520
5.190838-76-7 https://www.bicbiotech.com/product_detail.php?id=6521




